
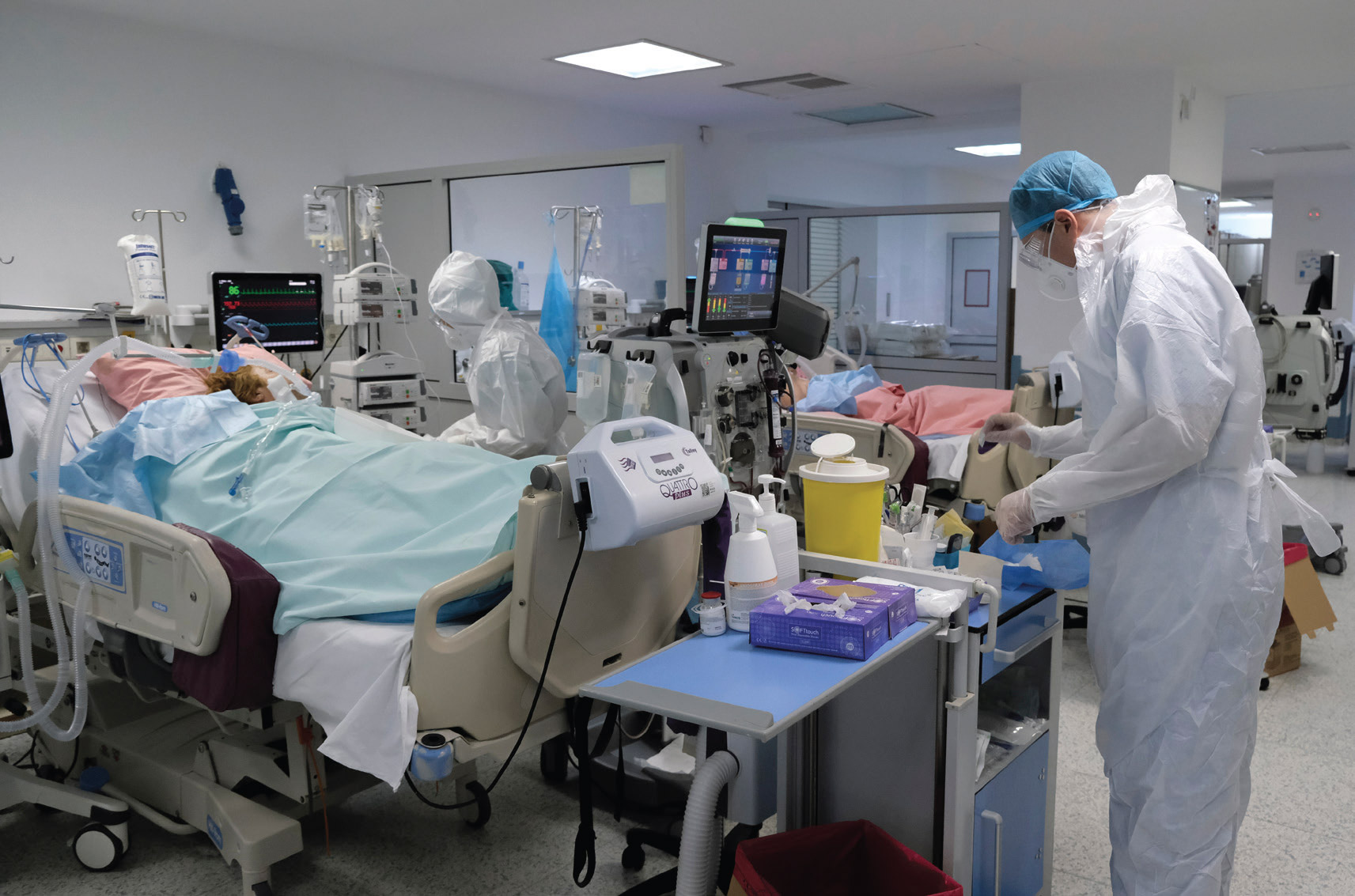
The infection risk present in hospitals has been a concern for hundreds of years. In the US, hospitals first introduced infection control as a formal discipline in the 1950s. Since the Covid-19 pandemic began in 2020, however, hospitals have been facing a level of infection risk they’ve never seen before. “Staff were inundated with patients,” says Dr Hilary Babcock, director of Infectious Disease Prevention and chief quality officer at BJC Healthcare. “Most infection prevention programmes really had to switch into sort of an all hands on deck response mode.” In practice, this meant hospitals had to make sure they had appropriate personal protective equipment (PPE) and the right kinds of isolation spaces for patients – all while educating staff on how to protect themselves and patients.
“[In Canada] Infection prevention and control (IPAC) became the main source of information during the Covid-19 pandemic, and the source of safety and control measures,” says Erica Susky, an infection control practitioner based out of Toronto. “Our role in communication became more crucial as new information and guidelines emerged from week to week, and sometimes from day to day.”
The risk of healthcare workers catching the SARS-CoV-2 virus that causes Covid-19 was a significant concern, and one shared by Babcock, who points out that healthcare employees live in the community just like patients, and when a wave of Covid-19 comes through, employees inevitably get sick, meaning hospitals have fewer staff during a spike. To further compound an already significant challenge, infection control practitioners had to maintain the infection control protocols required to tackle the usual suspects.
The reality of coping with all these demands was that the standard daily work of an infection prevention programme suddenly skyrocketed as practitioners struggled to find the capacity for their usual daily observations, audits and monitoring. “Our real challenge was in maintaining the standard practices we know are necessary to keep infections at bay, to be sure that not just the Covid-19 patients, but all the other patients coming through the doors for other things were protected and taken care of safely,” explains Babcock.
Other infections
Prior to Covid, hospitals were most concerned about device-related infections, such as catheterrelated bloodstream infections or catheterassociated urinary tract infections; surgical site infections; and clostridium difficile (C. Diff) – a bacterial infection that can result from antibiotic use. During the pandemic, numbers of these and other non-Covid-19 infections actually spiked. Hospitals are seeing more cases of central lineassociated bloodstream infections, but also C. Diff; fungal and bacterial pneumonia; and ventilatoracquired pneumonias. With Covid-19 in the equation, not only have these risks remained, they’ve become intensified. “Having Covid-19 can affect your immune system and the integrity of your lungs,” Susky explains. This may make patients susceptible to having superimposed pulmonary infections. And anytime someone is hospitalised with indwelling medical devices (like central venous catheters or ventilators), this increases infection risk, too. “People hospitalised for a greater amount of time remain vulnerable to hospital-acquired infections. Indwelling devices remain a potential portal of entry for infections as long as they are in place,” adds Susky. Babcock adds that with workers being pulled in multiple directions, important infection prevention tasks, like cleaning a central line, can go unfulfilled.
This is especially true if patients are lying on their stomachs for sanitary reasons and accessing indwelling devices like central lines becomes more difficult.
The ‘Great Resignation’
A major challenge throughout the pandemic, according to both Susky and Babcock, has been the impact that the extra demand has had on healthcare professionals. “Staff fatigue and resources are the biggest current struggles,” Susky says. In many cases, the experience of the pandemic has led to workers leaving the field entirely. One in five have quit their jobs since the beginning of the pandemic, leading the U.S. Bureau of Labor Statistics to dub the situation the “Great Resignation”.
While the number of employed healthcare workers has been going down, patient volumes have remained high, and Susky explains how this puts pressure on the healthcare system. “Covid-19 is not going anywhere and is still a transmission risk in hospitals, which demands further diligence from staff. Many healthcare facilities have shared rooms, and with increased patient volumes, hospital rooms will be at capacity which increases the risk of transmission.” According to Dr Babcock, hospitals have also struggled to “operationalise the things that changed.” Government requirements and recommendations surrounding the virus have been continually changing over the last few years. Hospitals and other healthcare organisations have needed to stay agile, taking these changes and weaving them into their operations as soon and as smoothly as possible. For example, when the vaccine was made available for healthcare workers, Dr Babcock explains how the university and healthcare system for which she oversees infection control needed to get all 45,000 of its employees to vaccine clinics. “[The clinics were] an amazing response, but it was a huge effort by the same people who were needed to be running things for the hospitals and doing things in the hospital.” Next, those same clinics needed to be open to the public. “All of those things had to happen while we still had to be taking care of all the patients in the hospital and taking care of our staff as well,” Babcock adds.
What’s next
With Covid-19 hospitalisation rates at a much lower level now than they were earlier in the pandemic, infection control protocols have been adjusted to prioritise pre-pandemic infection risks. “For the most part, the policies that we have [now] are not based on the underlying state of the patient as much as on our knowledge of the specific infection,” Dr Babcock says. Like any rule, there are exceptions to this one; patients that are immunocompromised, for instance, may take longer to clear an infection and need to be put in isolation. “In general, we’re focusing on how the infection is transmitted and how we can interrupt that transmission,” adds Babcock. Moving forward, Susky says, some tools will remain the same.
Hand hygiene, she points out, will always be the best way to prevent the spread of infections. But infection prevention and control are intrinsically evolving fields. “IPAC methods will always be changing as they are science-based, which is iterative. As new information and discoveries are made, IPAC measures will change to reflect that. We all witnessed those changes throughout the Covid-19 pandemic.”
Experts are constantly conducting research on infectious diseases, prevention and treatments. The Covid-19 vaccine is a result of that research. But novel infectious diseases and the further development of antibiotic resistance are an everlooming threat. There’s also the fact that infection control is not a perfect science. “The goal in infection control is to consider all infections as preventable,” says Susky. “However, there may be infections that could have been prevented in theory, but are not preventable in real life.” This is especially true when healthcare systems are dealing with challenges apparent prior to the pandemic, as well as those directly caused by it.
“The goal in infection control is to consider all infections as preventable. However, there may be infections that could have been prevented in theory, but aren’t in real life.” Erica Susky
“Big picture issues that are a challenge include shortages of infectious disease physicians across the country and that they are not evenly distributed,” says Babcock. “There are rural areas that may not have an infectious disease physician within hundreds of miles. That’s a challenge for hospitals that are working on infection prevention programmes.” On a lighter note, with hospitals now able to focus on more than just Covid-19, infection control practitioners like Babcock and Susky are able to turn their attention back to preventing other infections – working with staff to ingrain good practices and reliably incorporate them into the hospital workflow. “I think overall,” finishes Babcock, “things are starting to turn back in the right direction.”





